Family Stories & Minutes of Meetings
Faye's Story Facebook Link
Faye was born in January 2010 with Malignant Infantile Osteopetrosis (MIOP). The pregnancy and birth were all normal and nothing was suspected until she was 8 weeks old. We began to suspect she couldn’t see and she constantly had a runny nose. We were eventually referred to the Bristol Eye Hospital where we were told she had delayed vision development. When Faye was 4 months old her head began to get very large very quickly. She was rushed into hospital where she had fluid drained from her skull. After many tests Faye was finally diagnosed at Bristol Children’s Hospital with MIOP. Fortunately, she was able to have a Bone Marrow Transplant and has now got 100% donor cells from an anonymous donor. Faye is blind because her optic nerves were crushed by overgrown bone as she developed in the womb, she also has Hydrocephalus and other global developmental delays. Faye is now 12 years old and goes to a specialist education facility near her home. Although her development is delayed, there is support in place to provide her with an excellent education and we believe that nothing is impossible.




Imogen's Story
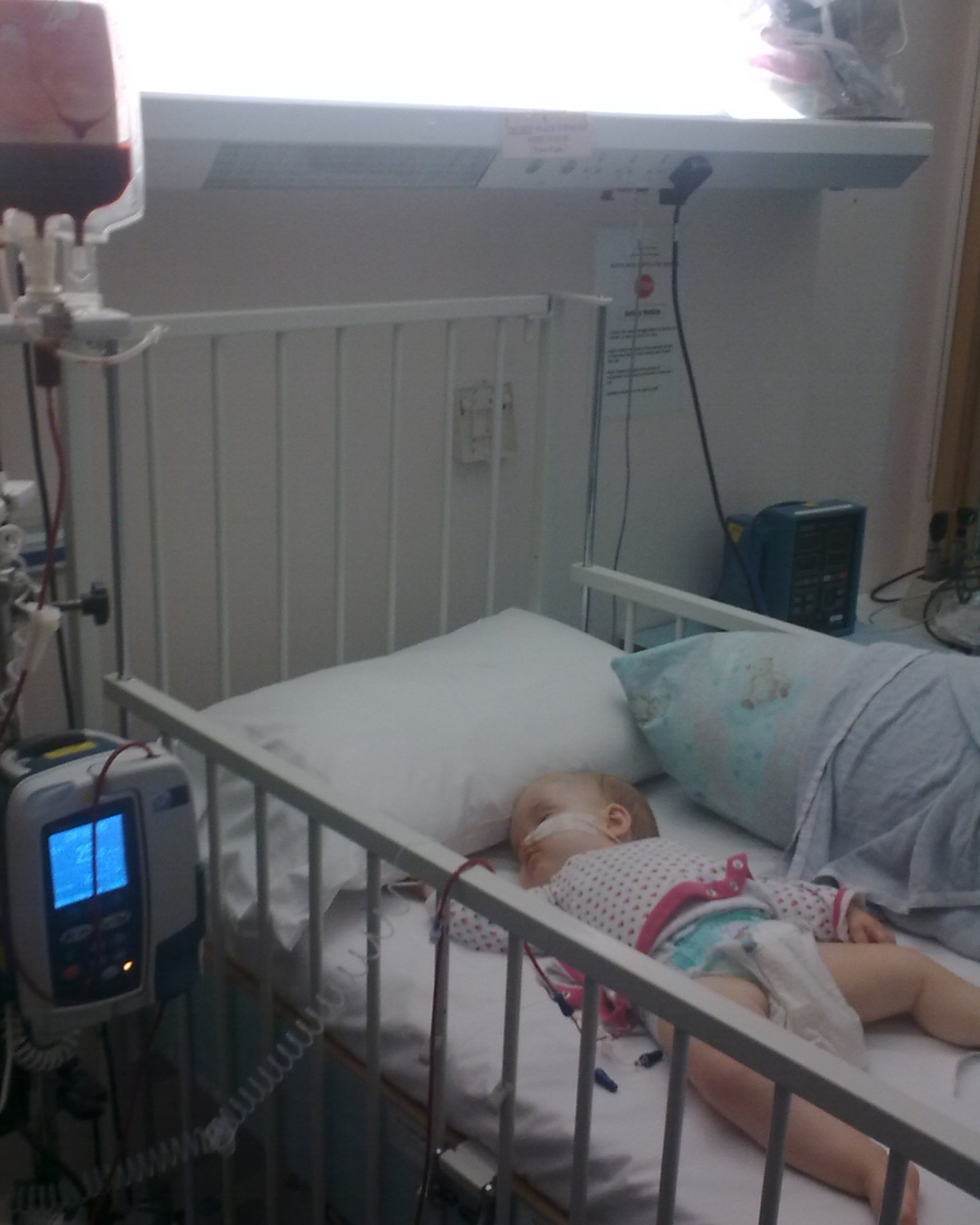
At about 8 weeks old we noticed Imogen's eyes were flickering and going cross eyed. When we mentioned this to the health visitor, she immediately got the doctor in. She was sent for scans as also her fontanelle wasn't quite right, and also saw an ophthalmologist. The scans showed nothing abnormal, but she was diagnosed with nystagmus. We saw a paediatrician every few months, and when she was 8 months old she had a blood test, and our Osteopetrosis journey began. 12th Jan 2011 we had the diagnosis at Bristol Childrens Hospital. A day we'll never forget.
Both of us, and our eldest daughter, then 3, were tested to see if we were a match. The best was 9/10. There wasn't a 10/10 match, and due to Imogen's rare tissue type there were only two others that were 9/10. It was decided that her Father, Alex, would be the donor. After several delays due to viruses, Imogen had her transplant September 2011 aged 18 months. It wasn't without its complications, but she was finally discharged in Jan 2012. Unfortunately, her level of donor cells declined slowly, and by Jan 2013, she was less than 5%. We made the decision to have another transplant. Luckily a donor was found who was a 10/10 match! 14th Jan 2014, she received the stem cells from a German female donor. She suffered from GVHD. After 4.5 months we were discharged, but once again the donor cells started to decline. She had a few stem cell top ups, but it wasn't effective. It was decided that a DLI, donor lymphocyte infusion, would be the only option . Previously, the t cells had been taken out as bizarrely JimJams levels were high. DLI had then still in. 3 months later we finally had the news she was 100% donor.
Imogen is totally blind, has moderate hearing loss and learning difficulties. At 11, she is getting stronger and taking tentative steps to walking. But what a happy little girl.

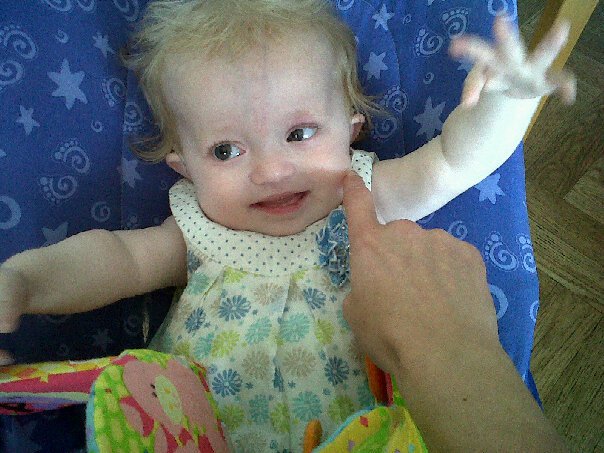



Alexander’s Story Written by Tracey Jones, Mum
Alex was born in 1993, my second son. His older brother, Matthew, then nearly three was delighted. During his first three months Alex’s weight gain was a little slow and he had continual snuffles. He then got a sticky eye. After several visits to our GP, Alex was thought to have an enlarged liver and spleen. The GP was concerned and said that there could be many causes for this including viral infections, blood disorders, etc. and we were admitted to Bristol Children’s Hospital where the Oncologist Consultant gave a provisional diagnosis of Malignant Infantile Osteopetrosis. He explained that Alex’s bones were “marbleising” as his bone marrow wasn’t functioning correctly. This was a rare genetic disorder but it was possibly curable.
We were told that the only possible treatment was a bone marrow transplant (BMT). There was a much better chance of success if Matthew was a match and we were told that there was a 25% chance of that. If he wasn’t, it was possible we might find an alternative donor, possibly myself or Alex’s Father (Chris) or from the national panel of potential donors. BUT… if the procedure was successful, Alex would be cured.
We were told that if a transplant wasn’t possible, the disease would progress and Alex would lose his sight and hearing, communication would become very difficult and then impossible. His brain would become cramped and damaged and he would be unable to fight infections. This would be because his bones would solidify and he would be unable to produce bone marrow. Without a transplant, he was likely to die before the age of 3. We were stunned at the severity of the condition and the poor chances of a cure. We went home.
Over the following weeks, Alex had many x-rays and blood tests. We all had blood tests to determine HLA typing (whether one of us was a match for the BMT) and at last I was told that my two children were perfectly matched. This was the best news I had heard for a long time. Alex was over his first hurdle.
Alex’s blood counts began to cause concern and he had a number of transfusions, both red cells and platelets. Some of these had to be carried out over long periods of time – because he was so small – and this meant staying in hospital.
There were major risks with the BMT; it was possible that Alex could die during or soon after the transplant. However, the hospital was very positive and gave us lots of information. We were talked through the drugs Alex would be given and the possible side effects and the antidotes given to counteract them. We were upset to learn that Alex would probably be rendered infertile because of the drug regime. It seemed a daft thing to be upset about, as if that was all he had to worry about in 20 years time – at least he would be around!
Alex had an ultrasound scan to ensure the major organs were healthy but this showed his right kidney was enlarged and blocked and also that his ureter was enlarged. He was injected with dye before special x-rays were taken showing his bladder and kidneys working.
Alex obliged – all over the Radiographer! The results showed a definite blockage around the ureter on the right side. Alex had surgery the next week to take the kink out of the ureter and attach it to the bladder in the right place. (This was seen as incidental and not associated with the Osteopetrosis). Alex’s surgery lasted three hours. When we were allowed to see him, he was wearing an oxygen mask and had two drips – one a maintenance fluid, the other morphine.
On the morning of Alex’s bone marrow transplant, Matthew had an operation to harvest his healthy bone marrow. Alex was in an isolation cubicle to protect him from infections. I had to change into sterilised clothes for the first time and observe isolation procedures. Matthew’s marrow arrived at the hospital mid-afternoon. I took a photo of the bag!! Matthew said, “That’s my blood going into Alex” and was very proud of himself. It was expected to take two weeks before a graft (when the new bone marrow is accepted by the new recipient) – it was going to be a long wait!
Alex’s white blood cell count dropped to zero and stayed there. He was “up and down” for the next week or so, needing the Total Parental Nutrition (TPN) to keep him going. His mouth was sore and he was unable to feed normally. Then his blood counts started going up… then down… but the trend was up. His chest became wheezy and there was some concern that he had another chest infection. Alex became lethargic and tired. The doctors decided, nearly three weeks after the transplant, that he was fluid overloaded and that his lungs were full of fluid. All but essential fluids were stopped and diuretics were given by what seemed like the gallon. Alex didn’t improve, in fact he got worse. He couldn’t breathe easily and his temperature and blood pressure were high. He was transferred out of the BMT Unit and into Paediatric Intensive Care Unit (PICU). We knew this wasn’t a good sign, he was still extremely vulnerable to infections and he had to change out of a clean environment into one where other people with germs were likely to be. However, within 36 hours we were back in the isolation cubicle on BMT where, strangely, I felt “safer”. Alex’s white blood cell counts continued to rise as well as his other counts and his need for blood transfusions diminished.
Alex left the BMT Unit less than six weeks after admission. What a wonderful and longed for day that was. Apart from a few minor hiccups, Alex’s recovery was remarkably good. He began to grow at a normal rate (although we were told he will never “catch-up”) and he has developed normally. He has no lasting sight or hearing problems.
As for the future, the prognosis is very good. Whether his fertility was affected remains to be seen. He must take Penicillin daily incase his immune system was damaged by the chemotherapy and this may continue for life. Otherwise he is completely normal. He plays football, enjoyed school and has a very outgoing personality – we consider ourselves very lucky.
Grant Funding for Sienna!
We were able to help Sienna in 2021 by providing funds to get her a good wheelchair to support her day to day life. Sienna was finding mobility progressively difficult and longer distances a challenge. Sienna's family applied for a grant via our website and we were happy to agree to support her. Doesn't she look fabulous in her new wheelchair!? This will help Sienna and her family enjoy getting out and about again and make life easier for travelling longer distances.

Minutes of Annual General Meeting - 12 February 2024
Meeting held via Zoom Video Conference
Present:
Secretary/Trustee: Sarah Sullivan SS
Chair/Trustee: Wendy Wilson WW
Treasurer/Trustee: Alex Wilson AW
Attendee: Michelle Edser ME
Apologies:
Trustee: Alison Gould AG
Trustee: Tracy Cubbage TC
WW opened the meeting and thanked everyone for being available.
Minutes of last meeting:
WW signed the last minutes as a true record of the meeting, passed by AW, seconded by SS.
Chair Report:
WW – 2022 to 2023 was a quiet year for incomings and outgoings. We fulfilled a grant request for a wheelchair. One grant request was refused for a sofa and fridge freezer, as the charity does not supply these items. No other requests were submitted.
Treasurer Reports – Financials Year Ending April 2023:
AW – had circulated the accounts to be approved in a previous email, all agreed the accounts were in order. The charity was financially sustainable. A donation had been made to Ryan’s bucket list and income had been received from a collection at his funeral.
SS – what was the actual OST financial year end? 30 April 2023?
WW – would check and confirm. The accounts were only just submitted on time.
Funding Requests:
WW - No new grant requests had been received, there was only one outstanding from last year. WW would contact the family and ask if they would like to update their request for approval.
SS – AP had said that a limit of £500 was set as a donation/grant amount years ago. Maybe this should be increased?
WW - thought that an amount had been agreed previously of £2000.
SS – there was nothing in previous minutes of any amount being agreed.
WW – OST Charity Constitution for giving grant payments:
1) The relief of sickness of persons suffering from Osteopetrosis.
2) The relief of poverty amongst persons suffering from Osteopetrosis and their families who are in need.
SS – could we amend the wording to say we support children and families with Malignant Infantile Osteopetrosis (MIOP), to be more specific?
ME – sometimes things should be provided by an OT or a council. Should be clearer on what we are able provide.
WW to investigate with the Charities Commission if we can amend the object of the charity and members to have a further meeting/email discussion as to what the objects should be now.
Communications/Social Media Updates:
WW – we should be adding something more to the Facebook page, periodically. When a child has a milestone, etc. Had an email from a nursing professional requesting information about families in the area but the area was not clear. WW had emailed to ask for clarification.
Any Other Business:
Charities Commission Log In
WW – the Charities Commission had changed the way to log in. ME and SS would log in and update their details. Would email an update to TC and AG to log in and set up themselves.
Osteopetrosis Awareness Campaign
WW – read out an email from Aseefa who has organised the Ostepetrosis Awareness Campaign. This was her own campaign and not a registered charity. She has the Dominant Osteopetrosis strain. Aseefa had requested to use the OST logo and collect donations on behalf of the charity in organisations such as Asda and other supermarkets. Permission from OST was needed.
ME – she could fundraise for us, but it seemed like it was making it complicated to handle charity donations. It was wonderful though, to raise awareness, using publicly available information. Would she be happy to contact OST for our bank details to forward any donations received? Would that be agreeable to Aseefa?
WW – would be happy for her to raise awareness and fundraise for OST but donations taken would need to be paid to the registered charity she was fundraising for.
AW – people raise funds at fun runs and send the donations onto charities, etc.
ME – if someone raised money for OST, could they set up a Just Giving page? Then send donations to OST directly. There was not one currently running for OST.
SS – yes, we have done that ourselves in the past but many years ago so there would be no current fundraising pages for OST.
WW would email Aseefa asking for more clarity in how she would be taking donations, etc. Unless she was purely raising awareness. More clarity was required.
WW thanked everyone for their time and closed the meeting at 8pm
Next meeting: to be organised for September 2024 – minimum of three Trustees needed for a meeting.